(WARNING: HIGHLY PERSONAL AND FRANKLY DESCRIPTIVE EXPLORATION OF MY BOOBS THEN AND NOW AHEAD.)
Many people mark the end of my cancer journey by the end of my chemo treatments. Not so. The end of this walk for me is when I get my boobs back. Sort of. Because I’m never going to really get MY BOOBS BACK, but I’m praying for a fair simulation at least.
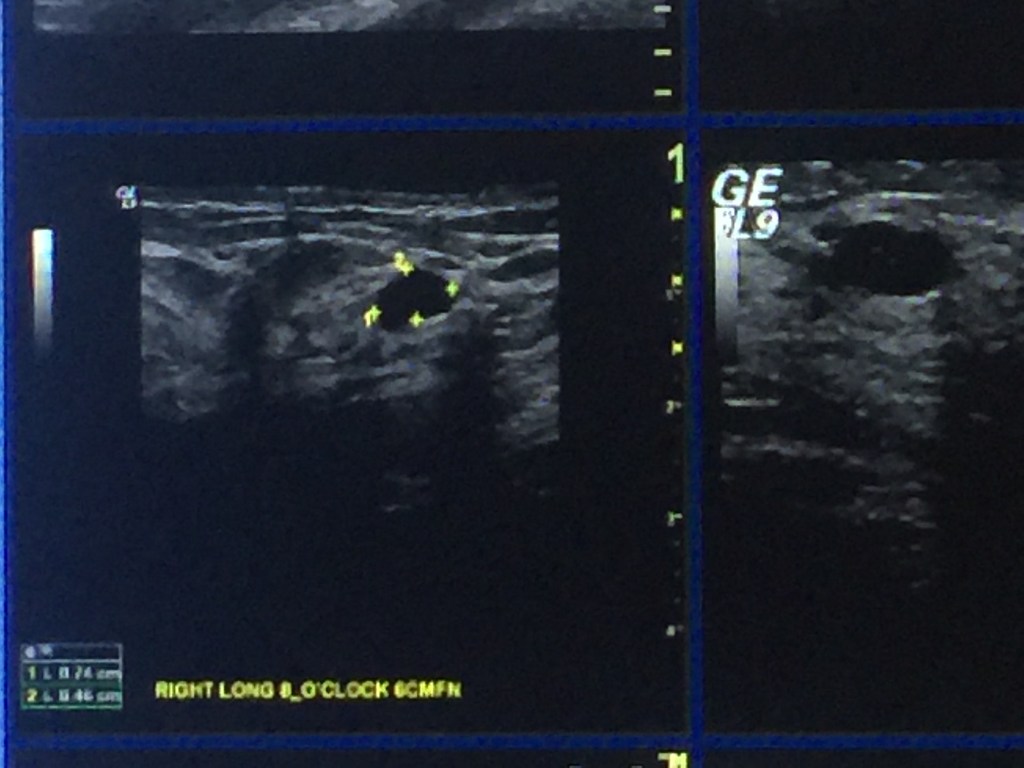
When all of this started, I wasn’t supposed to have a mastectomy, much less a double. Just a simple lumpectomy followed by months of small radiation treatments. If you’ve been following me, you know that many things changed along the way and my worst fears were realized when I was told I needed a radical mastectomy of my right breast. I then opted for the removal of my left breast because:
- With the multi-focal nature of my cancer and the difficulty we found in trying to diagnose the extent of my tumors (three surgeries–no reliable scans or tests beforehand) I never wanted to again question my mammograms, MRIs, biopsies and more should a problem arise in the left breast.
- Because of my former hefty, Playboy sized-boobies, removing only one would have created a near-impossible reconstruction task. By removing the other, I have a fighting shot at symmetry and balance, which is important to me.
I’ve said that from the start of knowing I’d need a chest castration (and YES, I do feel this way), that my only solace was knowing that I could end up with Perky C Cups, for the first time since I was 11.

Not my boobs. But they could have been.
If you remember some of what I’ve already shared, when I had the double mastectomy, we were not yet sure what kind of reconstruction I would have, because it was so sudden that I did not have time to finish my research and consultations with the doctors. So to give me the most options, my surgeon “installed” expanders–two pillow-like pockets that were placed behind my pectoral muscles. The purpose of the expanders is to slowly fill them with water to “expand” the skin they reside under until you get to the desired cup size. Then, the expanders are replaced with silicon implants. As the skin is already stretched from this slow process of increasing the water inside the expanders, the transition to implants is, ahem, seamless.
So I left the hospital with those expanders and several drains. But I had gone into the hospital with an active breast infection from the previous surgery. That infection, while being held at bay with powerful antibiotics, really never went away and three weeks after my mastectomy, I landed back in emergency surgery to remove the expanders. That was when I was at my lowest and sickest in all of this, and it’s an episode in my life I never want to relive. I was in so much pain I just wanted it to end, and I was almost delusional at that point, not realizing how much pain I was in. You hear about out-of-body experiences and this was mine, and not a good one.
But by that time I had decided that I wanted to do a very complicated reconstruction procedure called the DIEP Flap. Because I was going this route, I no longer needed the expanders, which is good because my surgeon, Dr. H, was now worried that I would never have fully been able to accept silicon implants.
The DIEP Flap uses fat from my abdomen to create new breasts. To do this, microscopic arteries need to be re-routed to my chest area to provide blood flow to my new boobs. It’s very complicated and definitely a specialty surgery, but the benefits are several.
- I would be using my own flesh to create my new boobs.
- There would be blood flow to the boobs, which means they would be an organic part of me. They would increase and decrease with my body’s weight changes, being more “natural.”
- I would be getting a tummy tuck (which I really don’t care about) at the same time since that’s where the fat comes from.
I really like the idea of NOT having something foreign in my body. To do this surgery, I face 2-4 days in the ICU, because the potential problems occurring from this surgery are so specific and require careful nurse monitoring, so they keep you there. Then there would be another outpatient surgery to “tweak” the boobs, to get them right. My understanding is that the boobs are not the issue. It’s the tummy work and artery re-routing that has to be carefully watched.
Had I chosen implants, that would be over several surgeries to get it all right, but none of them would be major. But I would always have to be vigilant about my new implant boobs. Silicon implants are not designed to be forever, one-time things. They have to be replaced over the years. And they have to be checked for leakage and other issues. I didn’t want that headache.
I don’t have the courage to take a picture of what I look like right now, but I do have the words to describe it. I have to first say that when you go through major, body-changing surgery like I have, and like so many other women have, you start to feel disconnected from your body. I often say that this is NOT my body. Between the chemo and the surgeries, it doesn’t feel like my body. It doesn’t respond like my body. It’s just not me. Reconstruction is about getting back some of me. I will never have all of me back; too many nerves were removed in this process. But I can at least enjoy the illusion of me, if it’s done right. I’m vain enough to want to have a nice, healthy, pretty body. I want my skinny clothes to fit again. I want to dress up and feel like a woman. Right now I accept that I don’t. I know it’s temporary, and the fact that my husband still loves me and wants me is what makes this bearable. But the hope of reconstruction is that I will again feel like me. Modified, but still me.
I have several friends and acquaintances who have consciously chosen for varied and personal reasons NOT to reconstruct after mastectomies. I honor and respect them for “living flat,” as they call it. That’s not me. I love the shape of my woman body, the curves and contours. I want as much of it back as possible, for me and no one else. For that I’m willing to be patient and to go through the pain and expense of reconstruction.
When I look at myself in the mirror topless these days, what I see is a blasted but neatly healing minefield where my boobs used to be. To preserve as much skin as possible for use later, my surgeon created skin pockets/flaps that were stitched in place under my armpits. They are not huge, but they are definitely noticeable when I’m undressed or wearing something tight, like I have football padding under my arms. The front of me looks nipped and tucked, with stitching lines where everything was sewn closed. Of course I have no nipples anymore. When the time comes, they will be “remade” by pulling up and sewing the flesh into little nips. Then they will likely be tattooed to give them color. (I kid you not.) The pictures I’ve seen show a good close reproduction of actual nipples and I can live with that. But I will never have feeling in them like the real things.
The sewn part of my chest is bumpy and I can feel my ribs just under the scars. Everything was sewn adequately to allow me to heal and get through chemo. We knew we were revisiting this whole area, so it’s neat, but not perfect nor fully symmetrical. I’m a little concave actually, and I’ve noticed that I walk differently. I have to consciously stand up straight, but without my boobs as a counterbalance, it feels different.
I did get prosthetic boobs several months ago. These are silicon inserts, fairly heavy, about a large B cup, that I can wear with a special bra. Wearing them is not about vanity, in this case. It’s about balance and weight. They are much smaller than what I sported before, but they do add some stuff for my clothing. Remember that our clothes are designed for boobs, even small ones, and the absence makes the lines of our clothes not hang right. In my case, since I don’t want to buy a new wardrobe yet (Be afraid, Stephen. Be very afraid!), I need to make my current closet work, especially my work clothes, which are more tailored. My prosthetics make this a little easier to do. And they help me stand straighter.
I’ve been very lucky in that while I certainly needed to lose a few pounds when all of this started, I had been working out regularly by August, and I was/am very flexible. Often, when we have mastectomies, there are more after-effects from the removal of our lymph nodes than the main part of the surgery. In this case, all of my nodes were removed from my right side, and tested (they came back clear which is the BEST possible news for breast cancer!). Just the removal and the tucking and stitching of all of the flesh in that area can cause us to not be able to use our arms freely. Range of motion is limited because you’ve taken away a lot of the skin that stretches with you. I’ve retained all of my range of motion, either because I was in good shape or my surgeon is that good. (Probably both.)
Because the lymph nodes help regulate the fluids in the body, I will forever more have to be careful about lymphedema, the swelling of the lymphatic system due to the removal of my nodes. I can no longer do anything which could trigger this condition, including having blood pressure taken on my right arm and having blood taken from my right arm. I have to wear compression sleeves anytime it’s needed and especially when traveling by plane (air pressure is the enemy here), and some other things I can’t remember right now. What a pain in my ass arm! But so far, it’s been workable.
Okay, so here’s the game changer in all of this. I’m open about the years of infertility we experienced to get Samantha. I wrote about it in a weekly column when I was still a reporter at the Ventura County Star back in 2000. Sam was 13 years in the making, and we lost nine babies before having her. All of our issues were on my end. I’d had a badly handled infection when I was 17 and the resulting scar tissue in my uterus closed my fallopian tubes. In response, I’ve had many, repeat many, surgeries to correct the tubes, remove tubal pregnancies, try to get pregnant and more. So many surgeries over so many years that my doctor and I can’t even put a hard number on them. But I guess between 20-24, most of them laparoscopies, but a few full-on laparotomies also, including my emergency C-section for Sam.
When my “Flap” surgeon heard this, he immediately stopped all conversation and wanted to know more about all of that abdominal slicing and dicing. Dr. W said that with all of that activity on my tummy, the likelihood of having damaged arteries is high. He called my infertility doctor, who has been with me for 28 years now, and was told laughingly that Dr. Jerry has so much written history on me, he doesn’t even have it all anymore. But that he would guess that yes, the arteries were damaged at some point in my quest for motherhood.
When I’m done with chemo, I will need to go in for an abdominal MRI. That will either completely rule out doing the Flap surgery, or it will send me under the knife with the potential for not being able to complete the surgery. The alternative is going back to the expanders and then to implants. Dr. W is not as concerned about my rejecting implants and expanders again. He believes it’s still an option, that the problems I had with them were specific to the infection and those surrounding circumstances.
For my part, I’m trying not to be discouraged here, but I’ll admit it’s really hard. And ironic.
After defeating so many years of infertility and having our precious daughter, I once again face the Spector of My Worst Battles. That’s right. For all that I’ve gone through with this breast cancer shit, I still believe that infertility was harder. Losing our babies, over and over, was the hardest thing I’ve ever gone through. This now is just about losing my boobs and curing cancer. I just don’t feel the same heartbreak as I do and did for my babies.

Nothing matters more in our lives than her. Nothing.
But I still want my boobs back. So, we’ll see. I’m very good about compartmentalizing my life and being patient. Right now, it’s all about chemo. Then it will be scan time. And then it will be decision and surgery time. I can do this.